Cleft lip, alveolus (socket within the jaw bone where the teeth are set) and palate
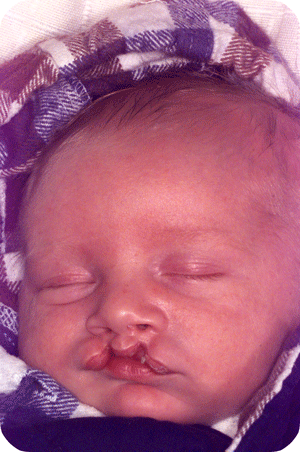
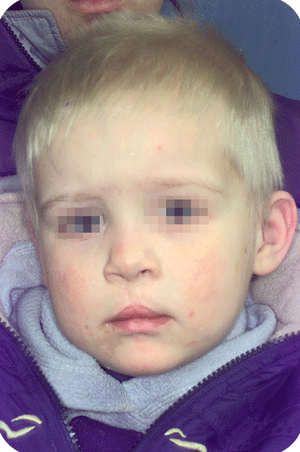
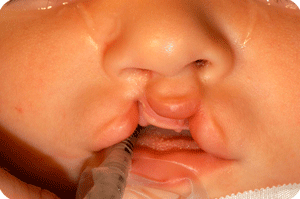
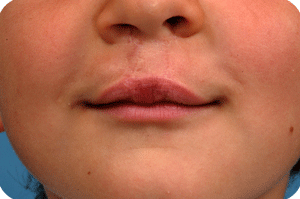
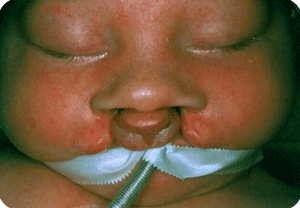
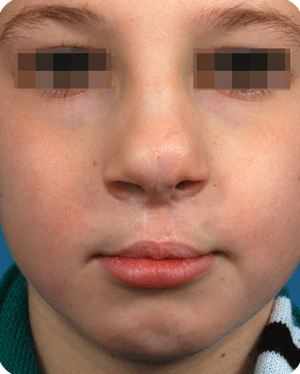
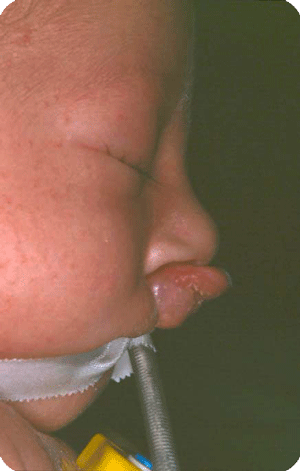
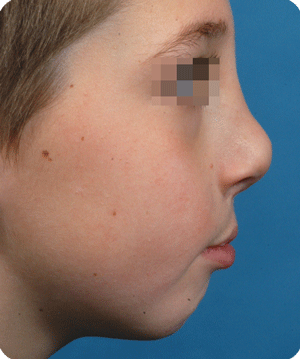
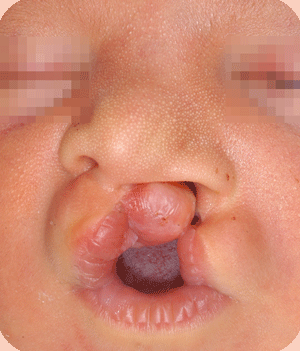
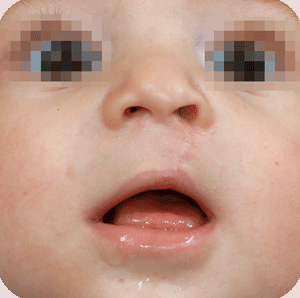
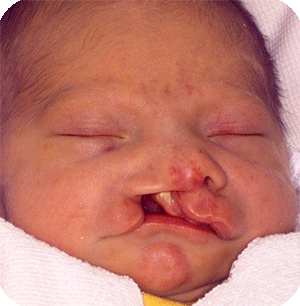
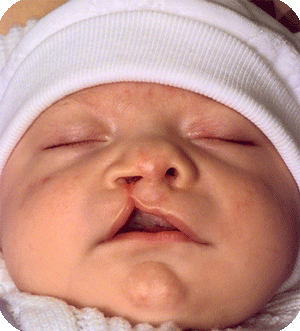
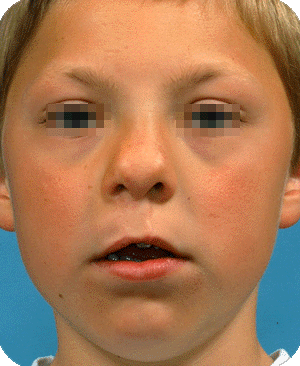
Cleft lip, alveolus and palate are the most common facial birth problems, affecting approximately one in every 500 to 700 infants. Complete facial rehabilitation for a child with a cleft abnormality generally involves more than the initial lip and palate repair. A multidisciplinary treatment approach from infancy through adolescence is necessary to achieve maximum success.
A complete cleft lip, alveolus and palate patient receives their first surgery in the third or fourth week. A preliminary lip and nose adhesion recreates an oral sphincter (opening of the mouth), although it is a primitive one. The delivered energy will move the small jaw forward and rotate the bigger segment backward to form a good platform on which the nose and lip can be reconstructed in a second surgery, at the age of four to five months. Guidance plate therapy is required to horizontalize the alveolus in the cleft area, in order to prevent the overriding of the segments and to lower the palatal shelves.
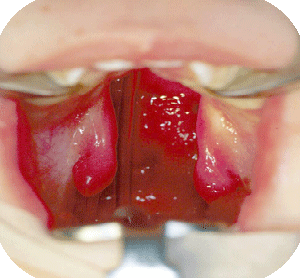
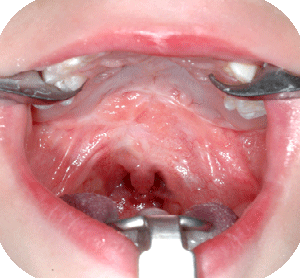
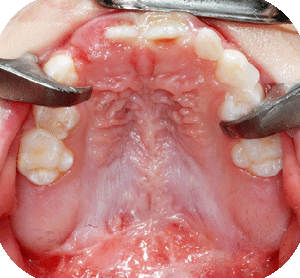
We prefer to close the palatal clefts, also when isolated, in two stages, to minimize growth disturbances by the development of unavoidable scar tissue. The goal is to reunite and reposition the velopharyngeal muscle slings, which have an important role in speech, hearing and swallowing. The hard palate cleft is left open till the age of four years, at which time transverse maxillary growth becomes stabilized.
Salvage surgery
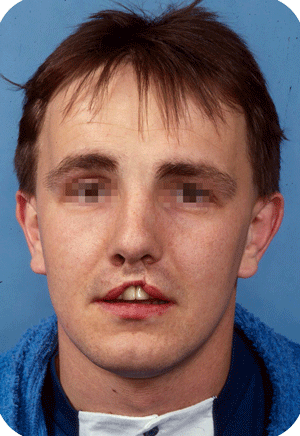

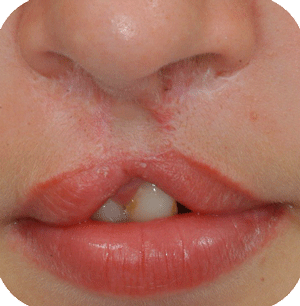
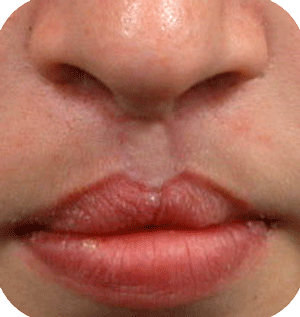
In Belgium, such deformations are not seen that often anymore, as cleft babies are transferred to cleft centres for their surgery. Secondary corrections are nearly always possible with acceptable results. The use of micorpigmentation (embedding of particles in the skin for corrective enhancement) can address small lacks of balance at the vermilion (around the lips) border.
Cleft nose
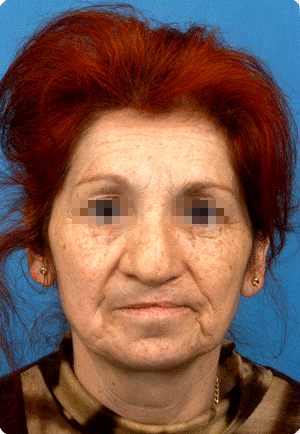

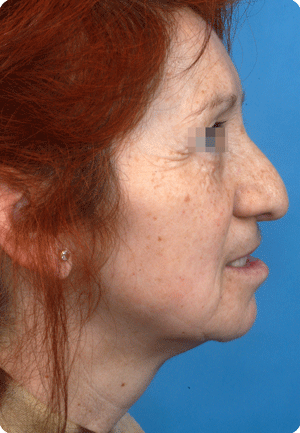
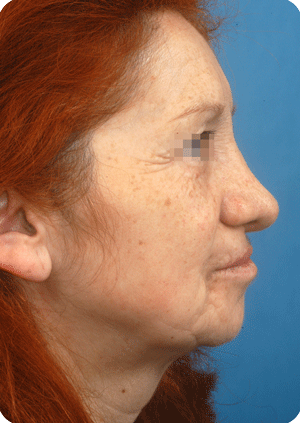
In bilateral clefts, earlier untoward columella (column in the nose ending at the tip) lengthening by a forked flap procedure has created a discrepancy in the nostril/tip area, which warrants corrections at a later age..
In unilateral clefts, the creation of balance is a challenge.
Craniosynostosis
Craniosynostosis (premature closure of one or more of the cranial vault sutures) affects one in every 2000 infants. One or more of the cranial vault sutures (coronal, metopic, sagittal, and lambdoid—all visual locations on the face) may be affected.
Reconstruction carried out by a craniofacial surgeon and paediatric neurosurgeon working together is essential to achieve sufficient brain decompression, to normalize the appearance, minimize morbidity and decrease the need for secondary procedures.
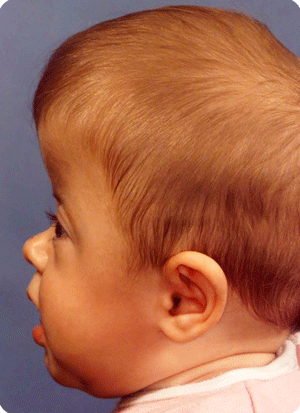
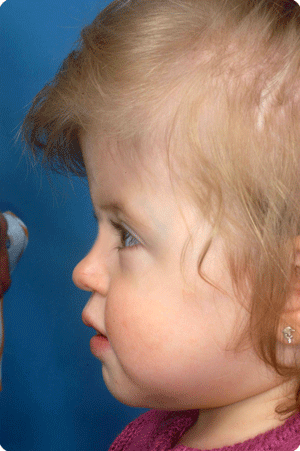
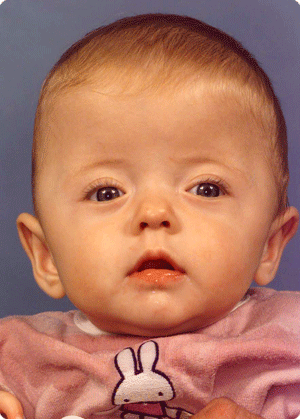
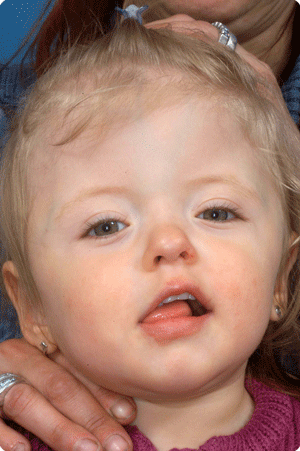
Other craniofacial malformations
Of the most common are hemifacial microsomia (condition present at birth that affects the development of the lower half of the face) and Treacher Collins (condition present at birth that results in downward slanting eyes, a small lower jaw and badly formed or absence or the ears), while Crouzon and Apert (both are a genetic disorder that affects the first pharyngeal arch, which is the beginning of the development of parts of the jaw) cases are more seldom.
Hemifacial microsomia is the second most common facial deformity existing at birth, after the cleft lip, alveolus and palate.
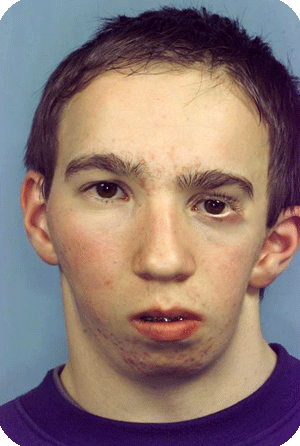
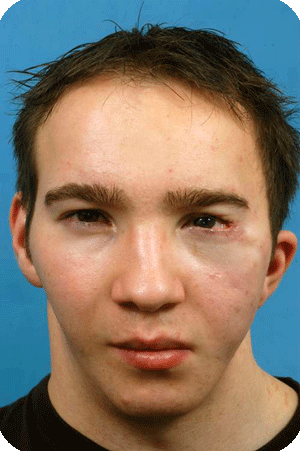
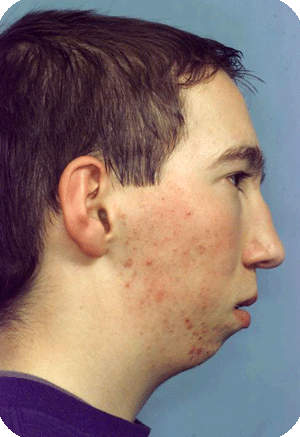
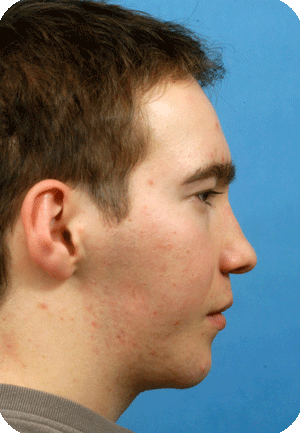
The spectrum is large, and the ears, jaws, soft tissues, nerves and eyes may be affected.
Facial rotation surgery with repositioning of the upper jaw, lower jaw, chin and eye sockets remains a challenge, even with modern 3D imaging techniques.
The cases may require phased soft tissue surgeries after the facial rotation (fat augmentation and eyelid surgery) and preliminary surgery to provide a functional joint with an abutting condyle, or to enable orthodontic treatment.
Crouzon syndrome
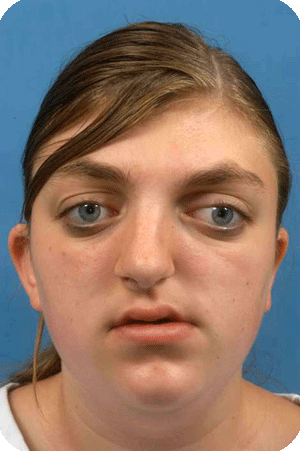

Le Fort III advancement procedure requires a coronal (over the head incision or open sky surgery). The midface as a whole is then advanced in one or two parts, to correct the prominent and endangered eye globes and to correct the anterior cross bite. Surgery may be required at a younger age when the eyes are exposed to trauma or when the airway is too small, or postponed till puberty to achieve a single stage, visually pleasing, and functional result in combination with orthodontic treatment.
| Back |



